Resources
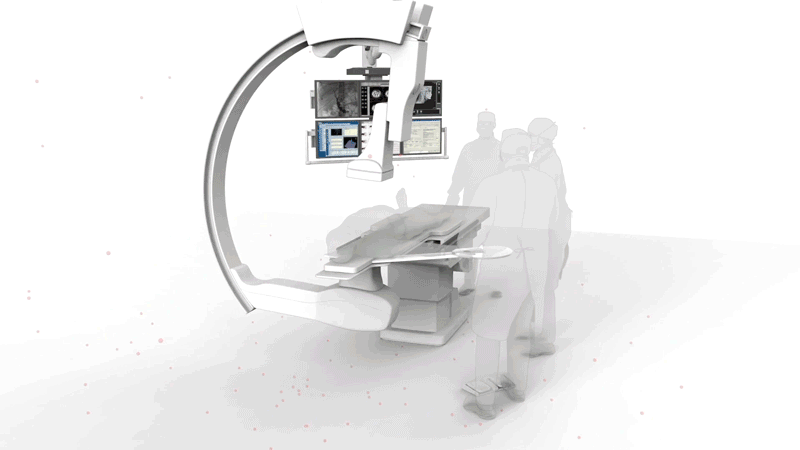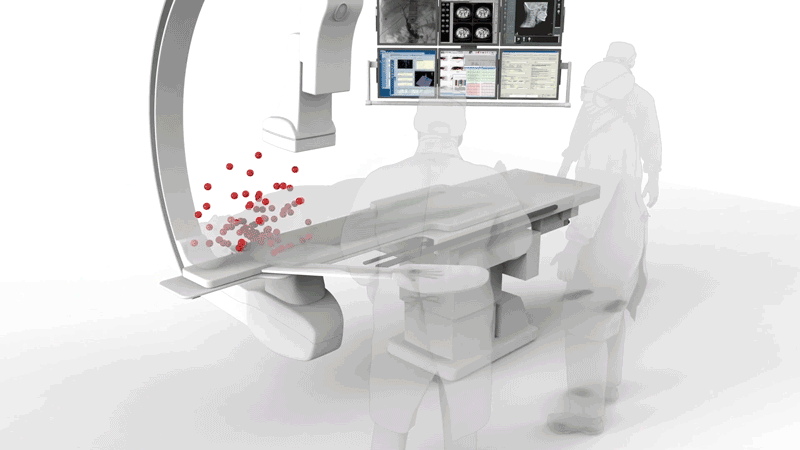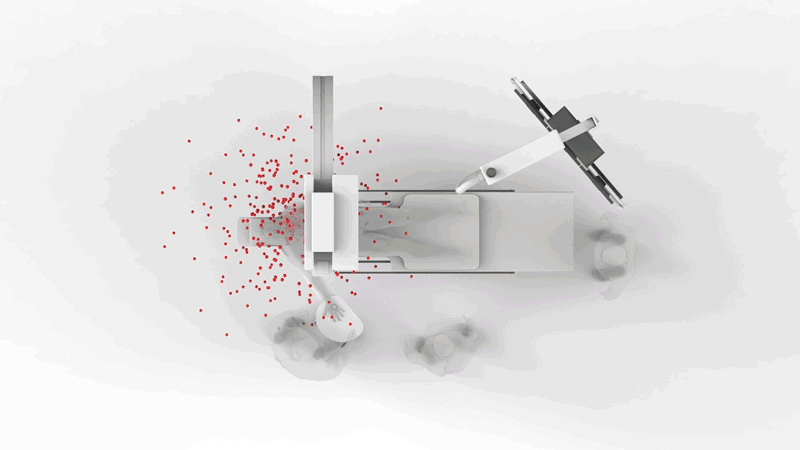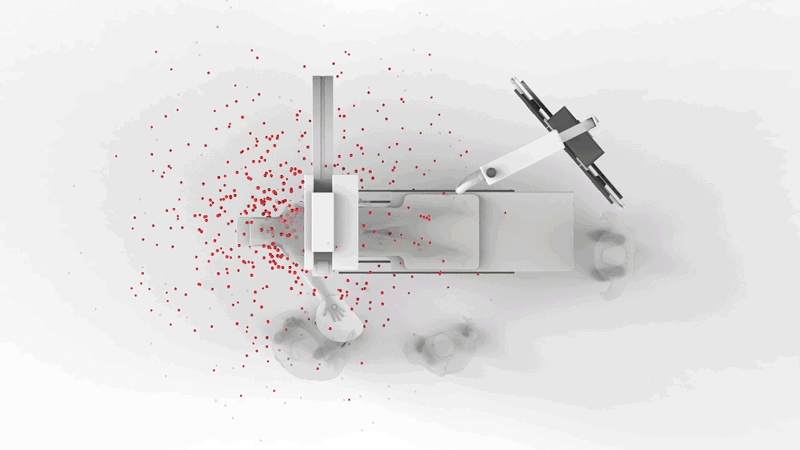
The resources in this section give an overview of the risks involved with ionizing radiation in the cath lab work environment.
With a FREE Membership to ORSIF, individuals can access even more resources such as resources, studies, white papers, videos, and community group to help connect, inform and minimize risk.
For organizations or businesses interested in supporting ORSIF, please click the button below to learn about our Corporate Member Levels.
Occupational Hazards:
Adverse Health Effects of Sustained Low-Level Radiation Exposure
Collection of data on the risk of adverse health effects caused by exposure to ionizing radiation is in an early stage, with most of the data coming from the studied effect on interventional cardiology teams. Mounting evidence shows a link to a series of significant stochastic health effects, including left-sided brain tumors, posterior subcapsular lens changes (a precursor to cataracts), skin cancers, thyroid disease, and neuro-degenerative disease. More generalized adverse health effects, such as cardiovascular disease and diminishment of reproductive capacity, also may be linked to general chronic, low-dose radiation exposure.1 Significant recent findings in these areas include:

ORTHOPEDIC INJURY
There is a significant risk that utilization of PPE can inadvertently cause debilitating adverse health effects in the form of spinal and other severe musculoskeletal and orthopedic conditions to the back, neck, hips, knees, and ankles.5 Surveys of cath lab cardiologists show staggering rates of orthopedic health impacts associated with the long-term, sustained use of heavy lead aprons while standing for prolonged periods of time to perform PCI and other interventional procedures.6

BRAIN TUMORS
It was once believed that the brain, unlike the eye or thyroid, is radio-resistant, and therefore not susceptible to the same effects as other more radio-sensitive organs.2 However, recent research has linked brain tumors, both benign and malignant, to low-level radiation exposure. For interventionalists who develop brain tumors, one study revealed that 85 percent of tumors originated on the left side of the brain.3

CATARACTS
The Occupational Cataracts and Lens Opacities in Interventional Cardiology (O’CLOC) study revealed that 50 percent of interventional cardiologists and 41 percent of cardiac cath nurses and technicians had significant posterior subcapsular lens changes, which are not age related and are typical of ionizing radiation exposure.4



REPRODUCTIVE HEALTH EFFECTS
For males, ionizing radiation has demonstrated a reduction in sperm.9 Medical professionals who may become pregnant while working in the cath lab must also take into consideration the effects that ionizing radiation can have on the developing fetus. Exposure to radiation in the first few weeks following conception can result in spontaneous expulsion of the embryo, and radiation doses of 1-2 Gy during fetal organ development could result in abnormalities.10
THYROID DISEASE
Studies have reported structural changes of the thyroid as a result of radiation exposure.7 Structural changes, such as malignant and benign thyroid tumors, develop at a linear rate to dose exposure.
CARDIOVASCULAR CHANGES
Recent studies suggest evidence of a link between low- to moderate-dose radiation exposure and cardiovascular changes, despite the proper utilization of PPE.8
U.S. Environmental Protection Agency Office of Radiation Protection Programs Home Page; Health Effects, http://www.epa.gov/rpdweb00/understand/health_effects.html (Accessed on November 10, 2014).
E Picano, et al, 2012.
A. Roguin, et al. Brain and neck tumors among physicians performing interventional procedures. 111 American Journal of Cardiology 9:1368-72 (May 2013).
E. Vano, et al. Radiation-associated lens opacities in catheterization personnel:results of a survey and direct assessments. 24 Journal of Vascular Interventional Radiology 2:197-204(2013).
D. Miller et al., Occupational Radiation Protection in Interventional Radiology:A Joint Guideline of the Cardiovascular and Interventional Radiology Society of Europe and Society of Interventional Radiology, ardiovascular and Interventional Society of Europe & the Society of Interventional Radiology (2010).
LW Klein, et al. Occupational Health Hazards in the Interventional Laboratory:Time for a Safer Environment, 20 Vasc Interv Radiol 147, 147 (2009).
E. Ron, R. Brenner, Non-malignant thyroid diseases after a wide range of radiation exposures. Radiation Research, 174:877-888 (2010).
E. Picano, Cancer and non-cancer brain and eye effects of chronic low-dose ionizing radiation exposure, BMC Cancer, 12:157 (2012).
A. Budorf, Effects of occupational exposure on the reproductive system:core evidence and practical implications, Occupational Medicine 56:516-520 (2006).
P. Best, et al, SCAI Consensus Document on Occupational Radiation Exposure to the Pregnant Cardiologist and Technical Personnel, 77 Catheterization and Cardiovascular Interventions, 232-241 (2011).
Economic Impacts:
Radiation Exposures Associated with Interventional Fluoroscopy

Minimally invasive treatment of many cardio-, neuro-, and peripheral vascular conditions has surpassed open surgeries driven by numerous benefits, including fewer major adverse events, shorter hospital stays, and faster recovery. These endovascular procedures would not have been possible without fluoroscopy, which provides real-time images of the location and movement of therapeutic catheters inside the body.
However, over the past two decades, there’s been increasing scientific and clinical evidence that chronic exposure to fluoroscopy, which emits low-dose ionizing radiation, is putting interventional medical professionals at risk for serious health conditions, including cancer.
To date, there has not been an economic analysis of the impact of these health-related occupational hazards. The Organization for Occupational Radiation Safety in Interventional Fluoroscopy (ORSIF) sought to quantify the economic costs associated with common health consequences of chronic exposure to ionizing radiation, specifically the development of cancer and orthopedic injuries. Based on the incidence of these adverse effects, ORSIF estimates the annual economic costs to be at least $49 million in the United States alone. This estimate excludes the treatment of non-acute medical conditions, such as precursors to cataracts, cognitive decline, and risks to reproductive health. It also does not account for turnover costs of experienced physicians nor potential litigation from physicians or patients. Absent investment in radiation exposure control technologies, economic costs will likely increase based on the continued shift to minimally invasive procedures.
Membership Options
Individual / Professional
Free Membership
It's FREE to join ORSIF as an individual. Create an account to gain access to resources and a members-only community of your peers. Enjoy access to a community of your colleagues, and benefit from professional resources such as educational resources, videos, studies, and other materials.
Corporate Supporter
Paid Membership Options
Align with esteemed companies and organizations engaged in interventional cardiology, fluoroscopy, electrophysiology and related fields. Whether your organization is an OEM, supplier, non-profit, association, or society, it is vital for operators in the space to come together to advocate for and promote radiation safety.